Go with your gut: this bacterium might be hiding in your stomach.
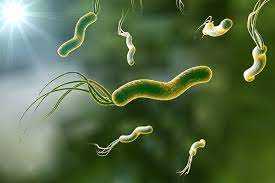
Your stomach is an incredibly harsh place. Its environment can reach a pH as low as 1.5 -- more acidic than a lemon. That’s strong enough to kill most bacteria, parasites and pathogens.
Of the handful of bacteria that do survive in the gut, microbiologist Mark Forsyth of the College of William & Mary in Williamsburg, Virginia studies Helicobacter pylori. His goal: to understand how the bacterium uses its genes to acclimate during its lifespan to the tough environment of the stomach and how, over time, it evolves to survive long term. The work could help develop new medical treatments for H. pylori, which can cause gastric ulcers as well as stomach cancer,
the fourth most common deadly cancer.
Forsyth is interested in a protein called ArsS that seems to affect how H. pylori senses and responds to the acidity of the stomach. ArsS has the unique ability to undergo both acclimation and adaptation at the same time.
“Acclimation” is how H. pylori directly reacts to changes in its environment. Experiments have shown that ArsS changes its activity depending on the acidity of its environment. In more acidic environments, ArsS seems to regulate the internal acidity of the H. pylori bacterium so that it remains stable. “Adaptation,” meanwhile, is a genetic process only able to occur across generations, such as by producing mutant forms.
How does H. pylori adapt over generations? One clue is when a gene contains a repetitive sequence of DNA that mutates over generations to activate or inactivate itself. This repetitive sequence is also found in the ArsS gene, but it does not activate or inactivate the encoded protein.
“It just changes the last 20 or so amino acids,” Forsyth explained. “It's weird. That is my albatross. That is the albatross around my neck. I've been trying for 23 years to figure out how that protein is involved in both acclimation and adaptation.”
Adaptations have allowed H. pylori to develop features that actually help its human hosts. Children with H. pylori tend to have a lower likelihood of developing diarrheal disease or asthma. H. pylori also combats acid reflux by suppressing the stomach’s acid production, thus decreasing the likelihood of a person to develop esophageal cancer. People who take antibiotics to treat H. pylori often require acid suppressants so that they do not develop this other form of cancer.
“So this is why to me, infectious microorganisms are so fascinating, because you think of them as disease causing, but at some level, some of them may actually have a beneficial advantage,” Forsyth said.
In some people, H. pylori begins to have a negative impact on their health in their mid-adulthood. It appears to be the sole cause of stomach cancer, and is a cause of stomach ulcers, typically resulting in one but not the other if symptoms are experienced. Yet, according to the NIH, only 1-3% of people infected by H. pylori will develop stomach cancer, and only 10% of people infected with H. pylori will develop peptic ulcer disease.
Due to the existence of antibiotics that can kill H. pylori, stomach cancer is less common in the United States compared to other cancers, though still causing more than 11,000 deaths in the US in 2020. Additionally, effective antibiotics can be hard to obtain and can cause harmful side effects. Researchers hope basic research like Forsyth’s could reveal better ways to battle the bacteria.
Though some antibiotics are effective against H. pylori, antibiotic resistance has been slowly rising. To combat antibiotic resistance, Forsyth hopes that his research could offer avenues to make new antibiotics or chemotherapeutic agents to attack the bacteria.
Along with his role as a scientist, Forsyth prides himself on being a professor and watching his students grow. He likens witnessing the growth of his students and their passion for research to lighting a fuse. “Maybe, just maybe, somebody is kind of turned into a research junkie, and they come up with some great discovery,” he says.














